Denver Burn Injury Attorney
A burn occurs when the skin and possibly the underlying tissue is damaged by an external source such as heat, electricity, chemicals, sunlight, smoke inhalation, or radiation. The cells in the skin die after being exposed to these sources, causing a sensation of “burning” in the victim. While most burns are relatively mild, severe burns are some of the most painful injuries to suffer due to the way the nerves become exposed and the long recovery time associated with the affliction.
According to the Center for Disease Control (CDC), over 450,000 people visit emergency rooms every year for burn injuries, from mild to severe. Of this nearly half a million, around 3,400 a year will die from burn injuries. Children are particularly susceptible to burns due to their inexperience with dangerous substances, but the highest rate of incidence occurs to young adults between the ages of 20 and 29. Three-fourths of the 40,000 burn injuries that require hospitalization are treated at the 128 burn centers operating in the United States.
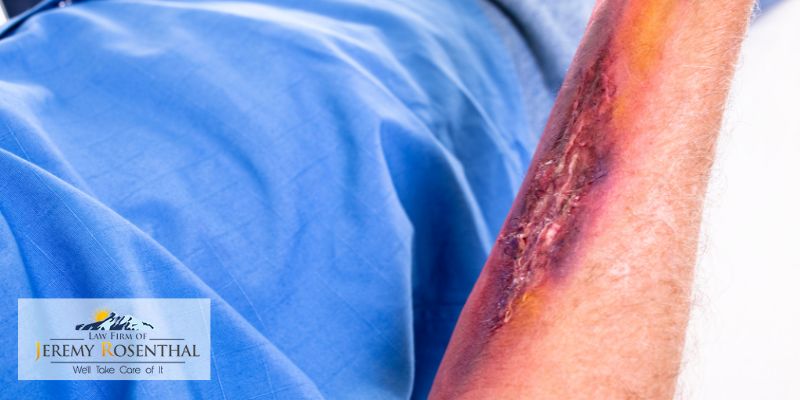
Burn Injury Classifications
According to the Center for Disease Control (CDC), over 450,000 people visit emergency rooms every year for burn injuries, from mild to severe. Of this nearly half a million, around 3,400 a year will die from burn injuries. Children are particularly susceptible to burns due to their inexperience with dangerous substances, but the highest rate of incidence occurs to young adults between the ages of 20 and 29. Three-fourths of the 40,000 burn injuries that require hospitalization are treated at the 128 burn centers operating in the United States.
As most people are generally aware, there are various degrees of burn injuries which designate the general severity of a burn. The damage done by a burn injury can also depend on how the injury occurred, the victim’s age and health condition, and other injuries that the victim sustains simultaneously, such as broken bones or internal injuries. The following is a general rubric that physicians use to evaluate burn injuries
First Degree Burns
First degree burns, also known as superficial burns, only affect the top layer of skin, such as a mild sunburn. In most cases, the injury will not cause blisters or scarring, although a person may feel feverish, and the area will hurt and possibly swell. The injury should heal on its own within a few days.
Second Degree Burns
Second-degree burns can be sub-classified as “superficial partial-thickness burns” and “deep partial thickness burns.” Superficial partial-thickness burns affect the first and second layers of skin and will blister and swell. Deep partial-thickness burns are not usually associated with increased pain, but rather with a sensation of pressure. The skin will appear spotted and waxy, and the area may become infected.
Third Degree Burns
Third-degree burns are also known as full-thickness burns because they damage all layers of the skin as well as the fatty tissue underneath the skin, inhibiting the body’s ability to regenerate skin. Third-degree burns may cause intense pain or may not immediately hurt at all due to nerve damage. The skin may blister, but the burn will likely be “dry, hard, and leathery-looking” and the color can range from white to black to bright red, or a combination. The risk of infection is particularly high.
Fourth Degree Burns
Fourth-degree burns are extremely severe. They are similar to third-degree burns in that they affect all the skin and underlying tissue, but they also extend through muscle, tendons, ligaments, nerves, and even bone. They require immediate and extensive medical treatment.
Different Causes of Burn Injuries
There are many different mechanisms of injury for burns, including thermal burns, cold burns, chemical, electrical, and radiation burns. Each mechanism requires slightly different treatment, and different types of burns have unique outcomes and protocols associated.
Thermal Burns
Thermal burns are the most common and include burns from scalding, direct contact with hot objects, and fire. Scalding occurs when someone is exposed to high levels of steam or hot liquid. These injuries are common in children and are often caused by spills, hot water from taps, draining pasta, or being splattered by hot oil while cooking.
Contact burns occur when someone comes into contact with something hot, such as a stove, coals from a fire, light bulbs, pipes, or pans. Contact burns often leave a pattern or mark on the body corresponding to the imprint of the object. Scalding and contact burns are usually first or second degree and will resolve on their own with at-home treatment.
The most common and dangerous thermal burns are caused by fire, which occurs in the home in the majority of cases. Burns can be especially bad if the occupant is trapped inside the house by fire or caved in ceilings. Thermal burns caused by fire are often associated with inhalation injuries, in which a victim is forced to inhale hot burning smoke from a fire which can damage the airway and/or lungs from both heat and toxic chemicals or particles present in the smoke.
Cold Burns
Cold burns occur due to extreme weather conditions, usually associated with frostbite, or by temporary contact with a very cold object. Frostbite ranges in severity, depending on the layers of skin and flesh that have been frozen. It may cause temporary numbness and pain, ulcers, blistering, or even the necessity for amputation in extreme cases. Ice packs (either gel, cold wrap, or bagged ice) can also cause first or even second-degree burns, especially since the cold can numb the area and the person might not feel the burn occurring.
Chemical Burns
Chemical burns, also known as caustic burns, can occur when your skin comes into contact with highly acidic or highly basic chemicals. If a chemical is swallowed, it can also potentially burn your internal organs, which is why you should always call poison control if you or someone you love swallows any non-edible substance. Common substances which cause chemical burns include pool chemicals, bleach, car battery acid, concrete mix, and metal cleaners. Incidents can occur inside the home or at work if a victim is exposed to chemicals on the job.
The severity of a chemical burn depends on many factors including the chemical’s concentration, the area contacted (whether or not it involves a mucous membrane such as the eyes or mouth), and the duration of contact, among other things. It is necessary to remove the chemical from the skin as quickly as possible. Victims may experience a range of symptoms from vomiting, pain, blisters, shortness of breath, numbness, or burning sensations to headaches, dizziness, seizures, or heart attack.
Electrical Burns
Electrical burns can fall into many categories including low-voltage, high-voltage, arc burns, oral burns, or flash burns, depending on the way the burn occurs. For example, oral electrical burns are usually suffered by children who put electrical plugs into their mouth or suck or chew on cords. Low-voltage burns occur when the victim makes contact with an electrical source of 500 volts or less, such as hairdryers, batteries, toasters, or vacuum cleaners. High-voltage electrical burns, on the other hand, involve contact with power sources such as electrical fences, power lines, and utility lines. Arc burns do not actually require contact between the victim and the power source because the electricity is so strong it can jump between objects, such as lightning.
The severity of an electrical burn depends on the strength of the current, the amount of time that the current was passing through the victim, and the part of the body through which the current passed. They are often characterized by “entry and exit wounds,” where the current made contact with the body. Symptoms of electrical burns include pain and/or numbness around the site of injury, confusion, headaches, dizziness, stiffness or muscle pain, and shortness of breath. Severe electrical burns can also be associated with cardiac arrhythmia and neurological damage. Electrical burns almost always require a visit to the doctor because there may be internal injuries.
Radiation Burns
The most common type of radiation burn is a sunburn. This is caused when the skin is overexposed to sunlight, which carries low doses of UV radiation. Malfunctioning tanning beds can also cause sunburns ranging in severity. Although most sunburns are mild and can be treated with cold showers, aloe vera gel, over the counter pain medication, and increased hydration, severe sunburns can occur after extended exposures. Severe sunburns are sometimes known as “sun poisoning,” although you are are not actually poisoned. In this case, symptoms may include extreme pain, blisters, swelling, and flu-like symptoms such as chills, fever, nausea, headache, and dehydration.
Other radiation burns can be caused by improperly administered X-rays or radiotherapy during medical imaging. They are also a common side effect of radiation as cancer treatment. Microwaves may also on occasion cause radiation burns.
Immediate Treatment
Treatment for burns should be immediate to prevent further damage to the skin and underlying tissue. For minor burn injuries, at home treatment should include extinguishing the source of the burn or removing yourself from the cause of the burn. With chemicals, you should immediately brush or wash them off. Burns should never be treated with ice because, although it numbs the pain, the cold will actually worsen the burn. Instead, treat with cold running water for an extended period of time, and cover the burn with a sterile dry cloth to prevent infection. Creams and lotions can create moist habitats to breed bacteria, so it is best to avoid them until recommended by a doctor.
Physicians will treat severe burns with a variety of techniques. This may include intravenous fluids to prevent hydration, prescription pain medication, burn creams, tetanus shots, and antibacterial drugs. In severe cases, the wound will need to be debrided, or cleaned of all objects in the wound and any dead or “necrotic” tissue. If the burn has affected your breathing, a surgeon may insert a tube into your windpipe to help you breathe and a feeding tube to provide nutrition.
Long-term Care
After the initial treatment, there are often other steps to take to ensure that a burned area heals and to reduce long-term scarring. Often severe burns require weeks or months of treatment in multiple stages which can be very painful and emotionally taxing. This may include skin grafts, taken from a donor or from pigs temporarily. Long-term problems associated with deep burns include the skin’s inability to sweat or to naturally moisturize the affected area, along with increased sensitivity to heat and cold.
Physical therapy is sometimes recommended to keep the body flexible and moveable. The new skin that grows over joints needs to be kept supple through stretching or it may be tight and restrict a victim’s movement. In addition, counseling may be recommended to help a burn injury victim cope with the mental trauma associated with the accident that caused the burn and the social stigma and psychological consequences of scarring caused by the burn.

Litigating Burn Injuries in Denver, Colorado
Like any injury caused by someone else’s negligence, victims can claim compensation for medical bills, past and future lost wages, lifetime care, pain and suffering and emotional trauma. A plaintiff must prove, however, that the burn occurred due to the negligence of another, either in maintaining their property or equipment or in manufacturing a defective or dangerous product. Because burn injuries are associated with high levels of pain, long recoveries, and permanent scarring, they often carry a higher settlement value, especially if the victim is a child.
Contact A Denver Burn Injury Lawyer Today
Burn injuries can happen in countless ways, from a chemical spill at work due to inadequate safety procedures, to a fire caused by faulty electrical wiring in the home. An attorney experienced in fighting for compensation for victims of burn injuries can greatly increase the chance for a positive outcome as they work to maximize your potential award. At the Law Firm of Jeremy Rosenthal, we will explore every possible avenue for getting you the compensation you deserve because we understand how devastating these kinds of injuries can be. Call us today at 303.825.2223 for a free consultation on your case or contact us online.
